An interview with Rebecca Edwards, Radiation Therapist Unit Leader
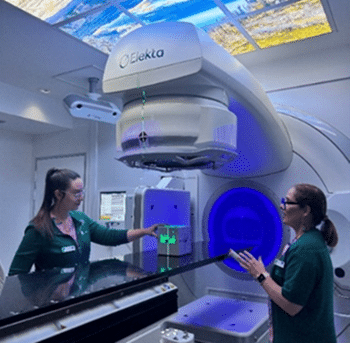
At GenesisCare South Australia in Adelaide, Radiation Therapist Unit Leader Rebecca Edwards and the broader clinical team are proving that surface guidance radiation therapy (SGRT) is more than just technology. It’s helping create smoother workflows and a more positive experience for patients.
 To explore how tattoo-free workflows are reshaping patient care and clinical practice, C-RAD spoke with Rebecca about her team’s experience implementing SGRT, the difference it has made for patients and staff, and what other centers can learn from their insights.
To explore how tattoo-free workflows are reshaping patient care and clinical practice, C-RAD spoke with Rebecca about her team’s experience implementing SGRT, the difference it has made for patients and staff, and what other centers can learn from their insights.
What do you find most valuable about using surface guidance in your radiation treatments?
I’ve been in radiotherapy for about seven years, so I’ve seen the transition from tattoos and markers to fully tattoo-free workflows. Being part of that evolution has been really rewarding. As therapists, we enter this field to make a difference through technology, and SGRT has been one of the most meaningful advancements in that journey.
Transitioning from snorkel-based DIBH to a fully snorkel-free, markerless, and contact-free approach has changed the experience for everyone involved. When patients finish treatment without permanent marks, it reinforces why this evolution matters.
Seeing patients’ complete treatment without permanent marks is powerful.
Patients also notice the difference right away with C-RAD’s Visual Coaching Light Panels. The color cues—green for correct breath-hold or positioning, blue for minor adjustments, and orange for stop or out-of-tolerance—help them stay engaged and in control throughout treatment. For therapists, that level of patient comfort and confidence is incredibly rewarding.
You’ve mentioned a priority for you is quality and process improvement. How has C-RAD supported that?
Quality and process improvement have always kept me engaged in this field. When we partnered with C-RAD, it wasn’t just about learning new technology—it was about shaping how it fit into our clinical practice.
- Strengthening collaboration between radiation therapists, physicists, and C-RAD experts
- Building structured learning and competency frameworks to keep skills current
- Rolling out progressively, starting with breast and DIBH before expanding to thorax, abdomen, and other treatment sites
How did you approach staff training and onboarding?
At first, it was a bit of a “thrown-in-the-deep-end” situation. But that was part of the learning curve! Over time, we built robust work instructions and a clear competency framework.
We started with a small core team who became confident and proficient before expanding training to others. Now, we have around 20 competent and another 10–20 proficient staff members who can train and lead SGRT workflows independently. That structure, combined with regular sharing sessions and documentation updates, has created consistency across sites.
What has SGRT changed most in your department?
It’s made our department even more patient centered. GenesisCare has always valued patient feedback, and SGRT amplifies that. Patients often tell us how meaningful it is not to be tattooed—and how much more natural it feels to breathe freely without a snorkel.
It’s also helped us improve efficiency. Using our OIS system (Elekta MOSAIQ) and internal Tableau dashboards, we’ve tracked detailed performance metrics and seen measurable improvements over time:
- Non–breath-hold breast: reduced from 12 minutes scheduled to 10.8 minutes actual
- Breath-hold breast: reduced from 15–18 minutes scheduled to approximately 13 minutes actual
Those numbers may sound small, but across a full day of patients the efficiency gain is significant. It means less waiting and better use of every treatment slot. We’ve also seen fewer re-images, reduced manual handling, and greater overall consistency with C-RAD solutions.
What differences have you noticed in staff well-being, patient safety, and overall treatment experience?
The reduction in manual handling is one of the biggest advantages. Before SGRT, therapists often repositioned patients by pushing, rolling, or realigning to tattoo points, leading to fatigue and an increased risk of error. With C-RAD, setup accuracy is visualized in real time, allowing millimeter-level corrections without unnecessary movement.
Now we rarely have to move the patient at all—sometimes it’s just a small hip adjustment of a few millimeters.
These improvements are most evident in three areas:
• Fewer repeat imaging sessions: Surface data provides immediate confirmation of setup accuracy before CBCT verification.
• Reduced physical strain: Staff who rotate to sites without C-RAD immediately notice the increased effort required. SGRT makes it safer for both therapists and patients.
• Greater patient engagement: Patients can see their own breath-hold in real time using C-RAD’s Visual Coaching Light Panels, which builds confidence and calm and leads to more stable, consistent accuracy.
We also use C-RAD’s color projection tools for quick postural checks. They provide an excellent visual aid when small corrections are needed before refreshing the image.
What treatment areas are you currently using SGRT for?
We started with breast and breath-hold breast, and now we’re using it for chest, lung, oesophagus, and abdomen. We’re also exploring faceless masks for head-and-neck patients, as well as SABR prostate and SRS. Long-limb setups, such as skin or extremity cases, are another area where SGRT could make a real difference.
The potential applications just keep expanding – anywhere precision and patient comfort matter, SGRT has a role to play.
Was it difficult to integrate SGRT into your existing workflows?
Not at all—we made it fit us. We adapted our existing processes, such as referencing the external and bony anatomy, and SGRT validated those setups with more information and greater confidence before imaging. We have real-time visual confirmation that everything is aligned before you even take a CBCT.
 How have your radiation oncologists and medical physicists responded?
How have your radiation oncologists and medical physicists responded?
Once they saw it in action, they were on board. Our radiation oncologists often mention that patients love the experience. It is calmer, faster, and more comfortable.
Working closely with physics has also strengthened our team dynamic. We’ve learned to see from each other’s perspectives, combining technical precision with human-centered care. That collaboration ultimately benefits the patient most.
Once you begin using SGRT, it’s hard to imagine working without it.
The key is to start small, build a strong core team, and let confidence grow through shared learning. Clear work instructions, peer-to-peer education, and collaboration with C-RAD’s applications team made all the difference for us. Today, our therapists work with greater accuracy and less manual strain, our patients are more comfortable and engaged, and our workflows are faster and more consistent.


 How have your radiation oncologists and medical physicists responded?
How have your radiation oncologists and medical physicists responded?
